A stepped care right care and treatment matched to a person’s mental health need approach is:
- a staged system of support options, ranging from the least to the most intensive
- is matched to a person’s individual and unique needs.
Ideally, care is provided early, in the least intensive and least intrusive way.
A stepped care approach offers multiple service options that match a person’s increasing and decreasing needs.
A stepped care approach aims to help a person access the right service to meet their needs at the right time and in the right place. It helps a person to stay well, or to sustain their recovery back to wellness.
Supports and services are offered to match assessments of symptoms and their impacts on a person’s daily life – on what a person is able to do from day to day.
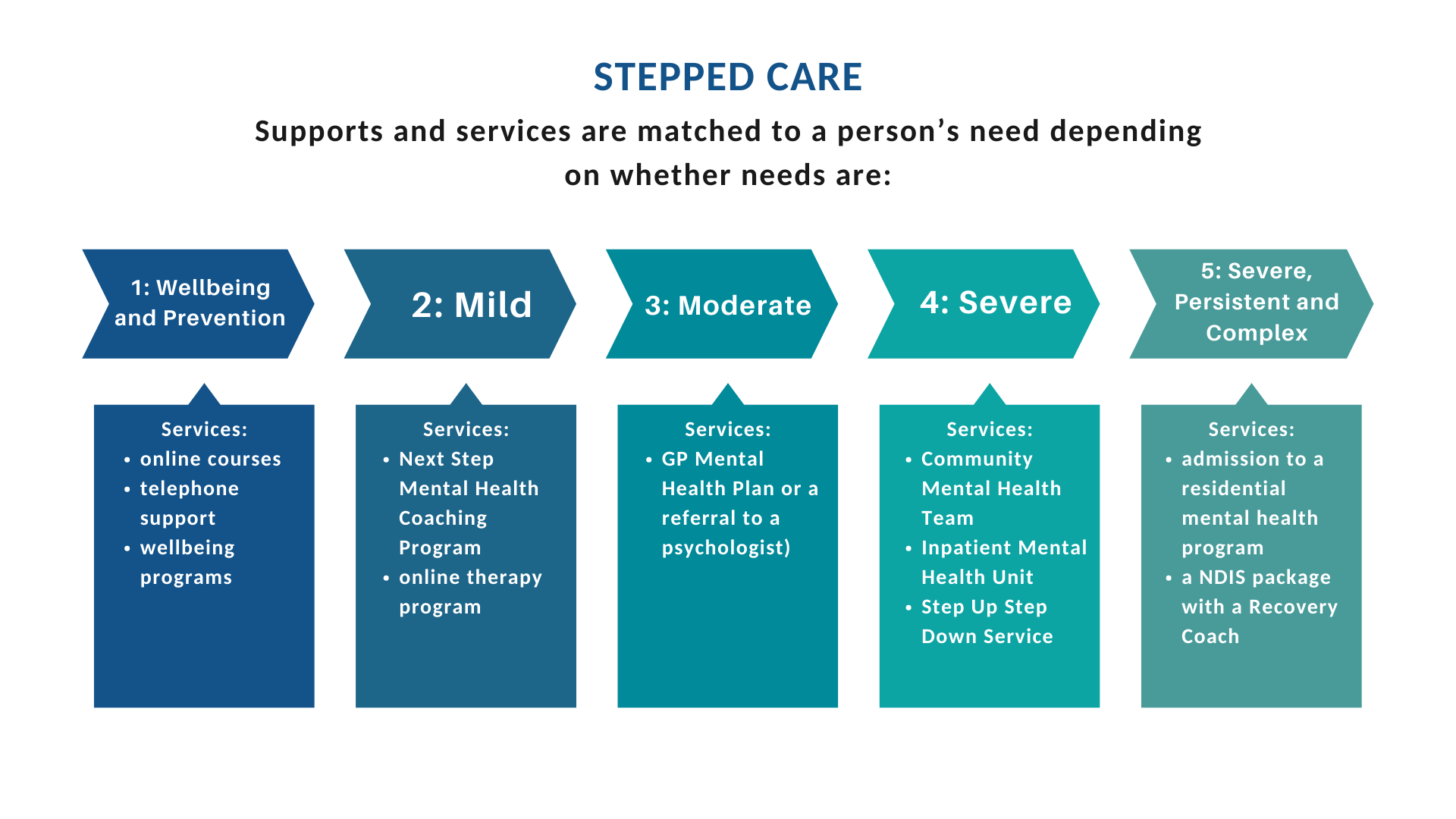
Depending on a person’s needs, support is provided through:
- directing people to self-help resources and support services
- online, eHealth technology and apps
- GPs general practitioner, local doctor, medical practitioner and health centres
- face-to-face support in a group or individual support, therapy and counselling
- care coordination with an Adult Community Mental Health Team
- Recovery coach and support coordination two support items provided through the NDIS for people with severe psychosocial disability
- medication and psychiatric review
- specialist mental health services – in people’s homes, the community and in hospital settings
- specialist psychosocial supports, peer support and disability support (e.g. through the NDIS or from a or community mental health support organisation)
The model considers the whole person and also addresses other needs including:
- physical health
- education and employment
- alcohol and other drug harm reduction
- family and social functioning and
- suicide prevention and self-harm reduction.
Emphasising collaborative care, the model involves a person’s GP, care team and significant others when appropriate. Services can be delivered by GPs, psychologists, social workers, occupational therapists, credentialed mental health nurses, psychiatrists, peer workers and other community workers and mental health workers.
The Mental Health Stepped Care model was introduced following the Australian Government’s response to the National Mental Health Commission’s review of programs and services in 2014.
-
What are the goals of stepped care?
The goals of stepped care are In a stepped care model a person seeking support receives services matched to their needs throughout their journey to help people access information. In stepped care, support and services are:
- Best suited and matched to their needs
- At the right time
- When and where it is needed
- As readily and easily as possible.
Importantly, stepped care means that support and services change as people’s needs change. As mental health needs change care and support can step-up (for someone becoming unwell) or step-down (for someone recovering from mental ill health) as required.
-
Who funds what?
The Australian Government takes responsibility for national policies, regulations, funding of health care, the delivery of primary health care Primary health care is the entry point to the health system. Your primary healthcare practitioner is usually your regular GP, who provides comprehensive and ongoing general medical care through Medicare and disability support including psychosocial disability through the NDIS.
The ACT Government is responsible for services through publicly funded inpatient services and community mental health, public health, ambulance and public dental services; and a range of mental health programs.
Primary Health Networks (PHN) – were established by the Australian Government to create a more integrated and efficient health system, including mental health. They do not deliver direct services, but they play a role in funding mental health and suicide prevention programs. They also have the role of helping create tools to help people navigate the system. In the ACT, the PHN is the Capital Health Network.
-
Who are the key service providers in the ACT?
Primary care – Most people access mental health support and services through their primary care provider, often their general practitioner or the local community mental health centre.
Primary mental health services – primary mental health services are the first line interventions. In the ACT they are funded by the Capital Health Network. Known as Next Step, people seeking support receive services matched to their needs on entry and throughout their journey.
Provided by Marymead CatholicCare, Next Step is a free program for people experiencing mild, moderate and severe mental health issues. Services are offered across a continuum by a trained clinical and non-clinical workforce. Benefits of the Next Step program include:
- free access and support for people who are unable to access other funded services where cost is a barrier
- evidenced-based structured intervention based on Cognitive Behaviour Therapy (CBT)
- online, telephone and face to face services in various locations across the ACT
- referrals accepted by individuals, GPs and other health care professionals.
If you would like to access their coaching program or don’t know which service is best suited for your needs, please contact their team on:
-
- Phone (02) 6162 6111 (during business hours); or
- Email NextStepIntake@mccg.cg.org.au
Other mental health programs funded by Capital Health Network– a range of specialised programs are also funded including
- Services for Aboriginal and Torres Strait Islander people
- Suicide prevention
- Child and youth specific services
- Services for people with severe and complex needs
- Services for underserviced groups
- Psychosocial supports.
Specialist mental health services – funded by the ACT Government, specialist mental health services are open to anyone who is seriously affected by their mental health condition and are provided in a person’s home and in hospital and community settings. They are accessed through
- Access Mental Health on 1800 629 354 or 02 6205 1065.
Access Mental Health is the central point of entry to access mental health services and are available 24 hours a day, 7 days a week. They will provide immediate information, advice, assessment and treatment (where required) if you or someone you care about is experiencing a mental health .
- In the event of an immediate, life-threatening situation for yourself or anyone else, always call ‘000’ emergency services first.
See the range of publicly funded specialist mental health services in the ACT.
National Disability Insurance Scheme (NDIS) – is the scheme for people with disability, including psychosocial disability Psychosocial disability is a term used to describe a disability that may arise from a mental health issue. Not everyone who has a mental health condition will have a psychosocial disability, but for people who do, it can be severe, longstanding and impact on their recovery. People with a disability as a result of their mental health condition may qualify for the NDIS. related to mental illness. To read more Mental Health & the NDIS :
The NDIS provides funding to enable people to purchase the reasonable and necessary supports they need.
Also important are the Disability Support Pension, Youth Allowance, Sickness Allowance and Carer Payments provided by the Australian Government and accessed through Centrelink.
Increasingly these services and supports are coming together to provide a spectrum of mental health options.
-
Statistics on Mental ill health in Australian aged 16 to 85 years
Mental ill health in Australian aged 16 to 85 years
- All adult Australians are likely to at some time will experience the need for wellbeing and resilience promotion
- 45% will experience a mental disorder sometime in their life
- Between 15 and 20% will experience symptoms and impairment in functioning sufficient to meet diagnostic criteria for a mental illness
- A further 23.1% will experience some sign of mental ill health or risk factors for mental illness, but will not meet the criteria for mental illness
- 9.0% will have mild disorders
- 4.6% will have moderate disorders
- 3.1% will have severe disorders, being all those with diagnoses of schizophrenia or bipolar disorder, and a proportion of those with other diagnoses such as severe depression where there are high levels of distress and functional impairment.
Of those with severe disorders (3.1%)
- two-thirds (2.2% of adults) have episodic disorders
- one third (1.1% of adults) have persistent disorders.
Over those with severe and persistent disorders (1.1% of Australians aged 16-85 years)
- Just over a third (0.4% of the population) will have significant functional and psychosocial impairment and complex multiagency needs.
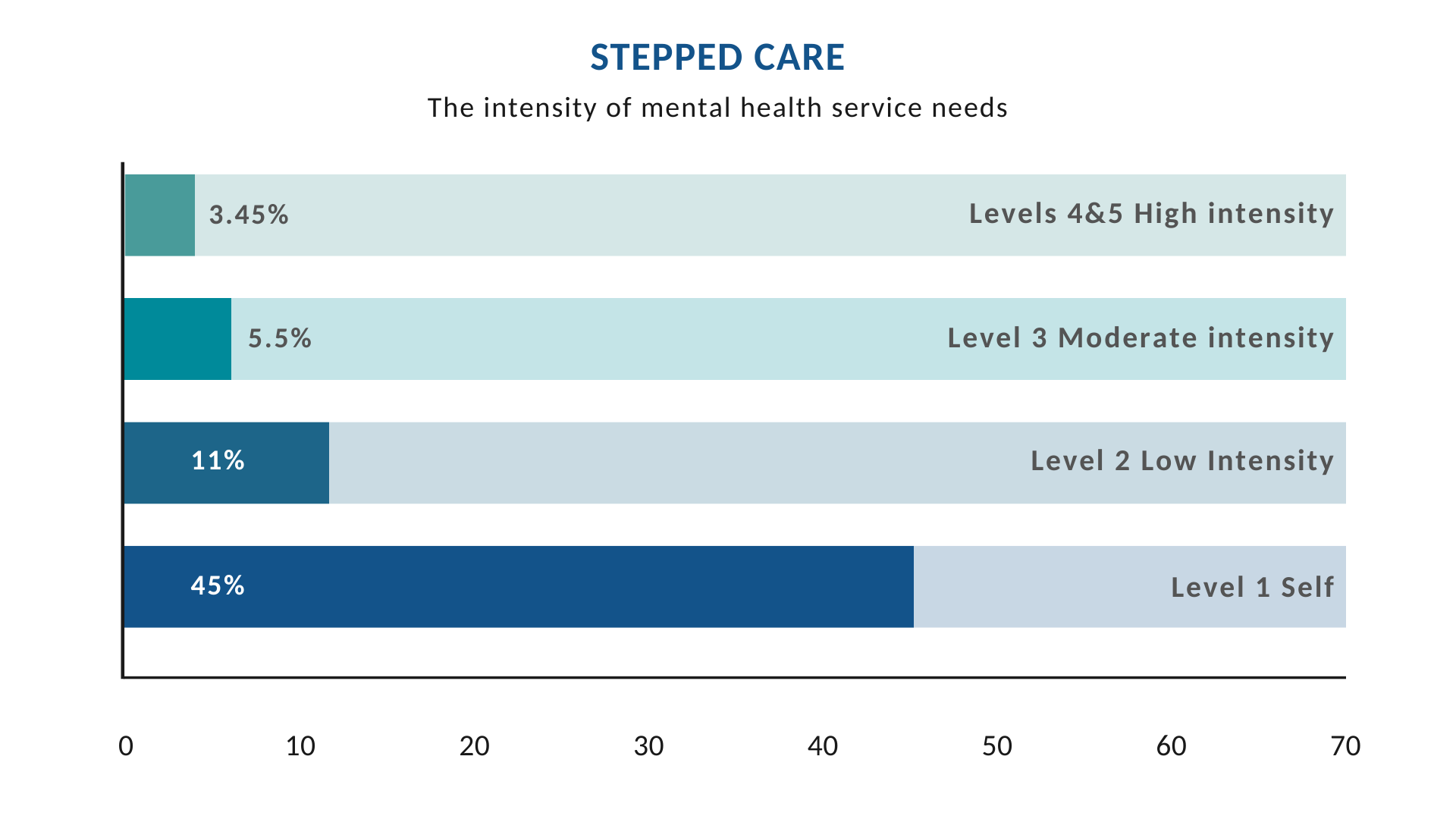
Most Australians with mental health issues and mental illness will access mental health services through their general practitioner or primary care provider. People who are seriously affected by their illness can be referred to the specialist mental health service system.
The chart below shows how the occurence of mental health needs falls within the stepped care spectrum.